
Endometriosis is a chronic disease of the female reproductive system characterized by the growth of endometrial tissue outside the uterus. Uterine fibroids are benign gynecological tumors caused by the proliferation of uterine smooth muscle cells with small amounts of fibrous connective tissue. Globally, the prevalence of endometriosis and uterine fibroids among women is estimated to be as high as 10% and 15–30%, respectively. While leading medical journals such as JAMA and NEJM have explored the potential health effects of these conditions, their impact on mortality has remained poorly understood. These disorders share similar pathogenic mechanisms and are often treated with clinical interventions such as hysterectomy, oophorectomy, and hormone replacement therapy, adding complexity to their analysis.
Recently, Dr. Yi-Xin Wang from the School of Public Health, in collaboration with teams from Harvard University, Michigan State University, Emory University, and other institutions, conducted a comprehensive study using a large, prospective cohort of women followed for over 30 years. This study examined the independent and combined effects of endometriosis and uterine fibroids on premature mortality and analyzed their interactions with lifestyle factors, hysterectomy/oophorectomy, and hormone therapy. The research revealed that laparoscopically confirmed endometriosis and ultrasound- or hysterectomy-confirmed uterine fibroids significantly increased the long-term risk of premature mortality from tumors, particularly gynecological cancers. Furthermore, endometriosis was linked to an increased risk of premature death from non-cancer diseases such as respiratory and neurological conditions. Women with both endometriosis and uterine fibroids were also found to have a higher risk of premature death from cardiovascular diseases.
The World Health Organization defines "premature mortality" as deaths occurring between the ages of 30 and 70. Since the release of China's Healthy China 2030 blueprint in 2016, improving early detection and treatment rates for common diseases among women has become a critical public health goal. Premature mortality in individuals aged 30–70 has significant societal impacts, as this age group represents a vital portion of the workforce. Losses in this demographic could severely affect productivity and hinder sustainable development.
In recent years, Dr. Wang's research in reproductive epidemiology has innovatively focused on premature mortality (deaths before age 70) as a health outcome. Her series of findings have demonstrated that reproductive-related conditions, such as menstrual irregularities, spontaneous abortion, childhood sexual abuse, gestational hypertension, gestational diabetes, and infertility, increase the risk of premature death. This study further confirms the influence of endometriosis and uterine fibroids on premature mortality, providing novel evidence to guide comprehensive women's health management throughout their life course.
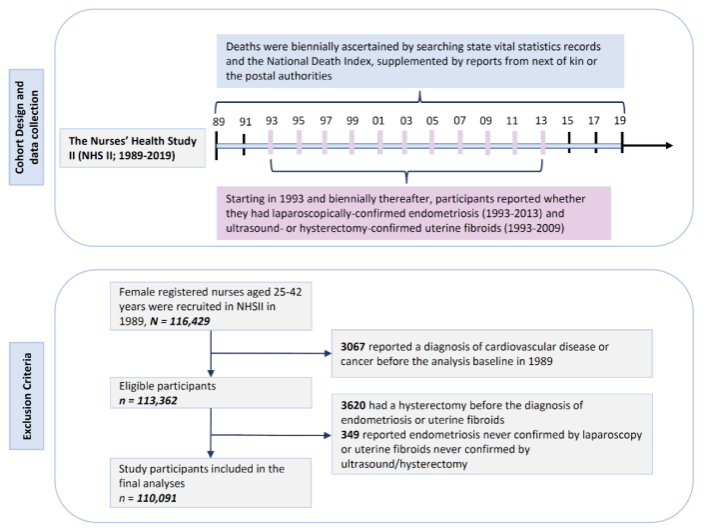
The research population was drawn from the Nurses’ Health Study II (NHSII), launched in 1989, which recruited 116,429 female nurses aged 25–42 (mean age: 34.7±4.7 years). Participants were followed biennially through mailed or electronic questionnaires that collected detailed data on reproductive traits, lifestyle factors, and health status. From 1993 onward, participants were asked biennially about laparoscopically confirmed endometriosis and ultrasound- or hysterectomy-confirmed uterine fibroids. To ensure data reliability, Professor S.A. Missmer's team validated self-reported diagnoses of endometriosis and uterine fibroids against clinical records in 1994 and 2011, finding over 93% consistency. For this study, individuals with baseline cardiovascular diseases or cancer (3,067), those who had undergone hysterectomy before diagnosis (3,620), and those without confirmed diagnoses (349) were excluded, resulting in 110,091 participants.
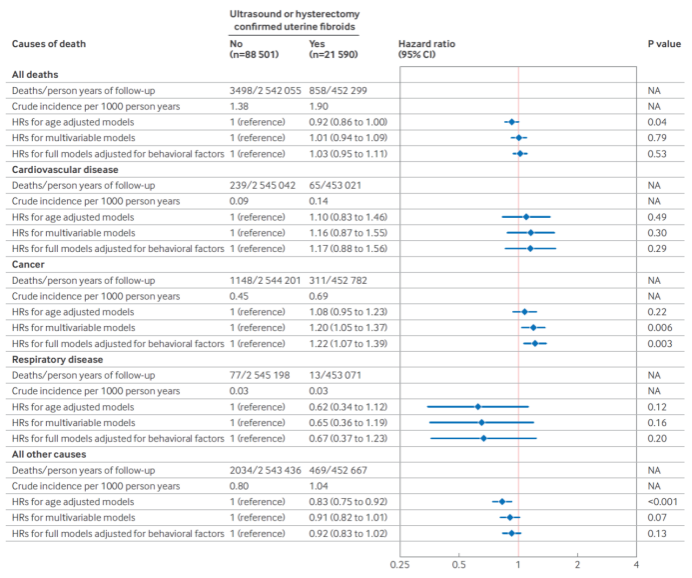
During the 30-year follow-up (1989–2019), the study documented 4,356 premature deaths, including 304 from cardiovascular diseases, 1,459 from cancer, and 90 from respiratory diseases. Women with endometriosis had a significantly higher crude mortality rate than those without (2.01 vs. 1.40 per 1,000 person-years). The hazard ratio (HR) for all-cause mortality was 1.19 (95% CI: 1.09–1.30), which increased after adjusting for confounding factors and lifestyle (HR = 1.31, 95% CI: 1.20–1.44). Cause-specific mortality analysis showed an increased risk of death from cancer (HR = 1.22, 95% CI: 1.04–1.44), respiratory diseases (HR = 1.95, 95% CI: 1.11–3.41), and neurological diseases (HR = 2.50, 95% CI: 1.40–4.44) among women with endometriosis. For uterine fibroids, no significant association with all-cause premature mortality was found (HR = 1.03, 95% CI: 0.95–1.11). However, the condition was linked to an increased risk of death from cancer (HR = 1.22, 95% CI: 1.07–1.39), particularly gynecological cancers (HR = 2.32, 95% CI: 1.59–3.40). Women with both conditions faced a higher risk of cardiovascular-related premature mortality (HR = 1.61, 95% CI: 0.93–2.76).

There was no significant association between uterine fibroids and overall premature mortality (HR = 1.03, 95% CI: 0.95–1.11). However, cause-specific mortality analysis showed that uterine fibroids increased the risk of cancer-related premature death (HR = 1.22, 95% CI: 1.07–1.39), particularly death from gynecological cancers (HR = 2.32, 95% CI: 1.59–3.40). Compared to women without either gynecological condition, those with both endometriosis and uterine fibroids had a higher risk of premature death from cardiovascular diseases (HR = 1.61, 95% CI: 0.93–2.76). Further stratified and interaction analyses suggested that the association between endometriosis and premature mortality was not influenced by factors such as race, diet, smoking, BMI, physical activity, hormone replacement therapy, infertility, spontaneous abortion, menstrual irregularities, oral contraceptive use, or aspirin use, indicating that endometriosis is an independent risk factor for premature death. Interestingly, among women with a history of hysterectomy, uterine fibroids were associated with a reduced risk of both overall premature mortality and cancer-related premature mortality. This finding suggests that hysterectomy may mitigate the progression of uterine fibroids to cancer, thereby lowering the associated mortality risk.
Dr. Yixin Wang from Shanghai Jiao Tong University's School of Public Health served as the first and corresponding author of this study. Co-authors included Professor J.E. Chavarro (Harvard T.H. Chan School of Public Health), Professor S.A. Missmer (Michigan State University), Dr. K.L. Terry, Dr. S. Wang, Professor A.J. Gaskins (Emory University), Professors J.W. Rich-Edwards and K.M. Rexrode (Brigham and Women’s Hospital), Professor L.V. Farland (University of Arizona), and Professor R. Tamimi (Weill Cornell Medicine, Cornell University).




